Food as Medicine: An Old Idea Made New
The notion that food is medicine is a familiar idea. Its recorded origins go back to the Ancient Greeks, where no less than Hippocrates himself is credited with saying “Let thy food be thy medicine and medicine thy food.”
Today, we are told that certain foods are “super” and can protect us from various ailments.
Fermented foods support gut health. Compounds in dark chocolate protect cells from inflammation. High protein diets boost metabolism. Flavonoids in berries boost memory. Omega-3 fatty acids in salmon improve mood and reduce symptoms of anxiety.
We’re also told that limiting or avoiding certain foods is an important part of managing certain health ailments once they’ve developed.
For people with diabetes, managing how much carbohydrates we eat is central to glucose management. When it comes to cardiovascular health, we are advised not just to limit the overall amount of fat we eat, but to avoid certain kinds of fat altogether. For hypertension, salt consumption can be problematic. For kidney health, we are told to limit sodium (salt), cholesterol, fat, and red meat.
All of this advice can be overwhelming. Sometimes it’s contradictory. Other times it comes across as more of a marketing message for a particular food product than health advice based on medicine or science.
The Academy of Nutrition and Dietetics (the world's largest organization of nutrition and dietetics practitioners) took aim at this confusing situation in 2021 when it adopted an official, science-based definition of Food as Medicine (FAM).
Food as Medicine, Officially Defined
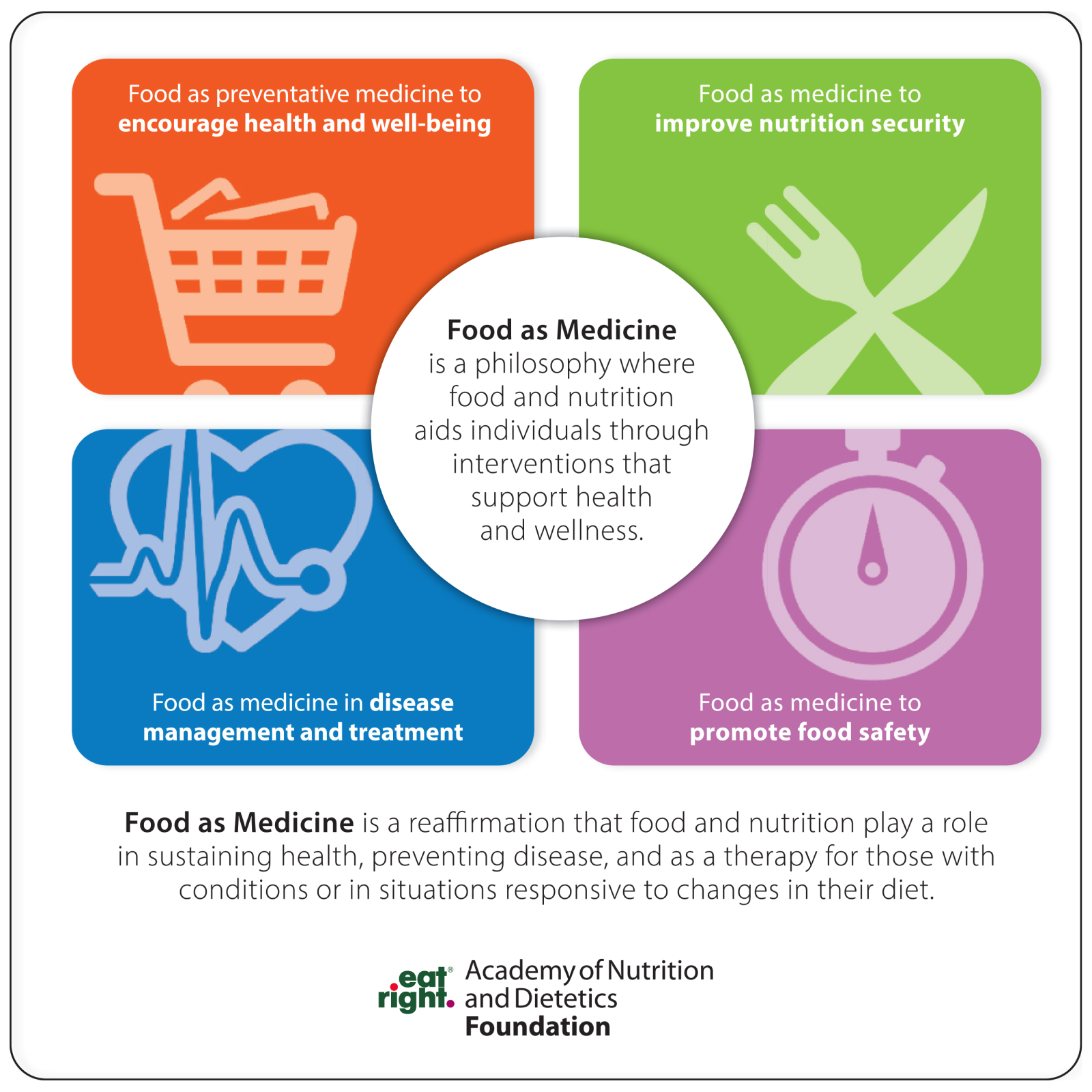
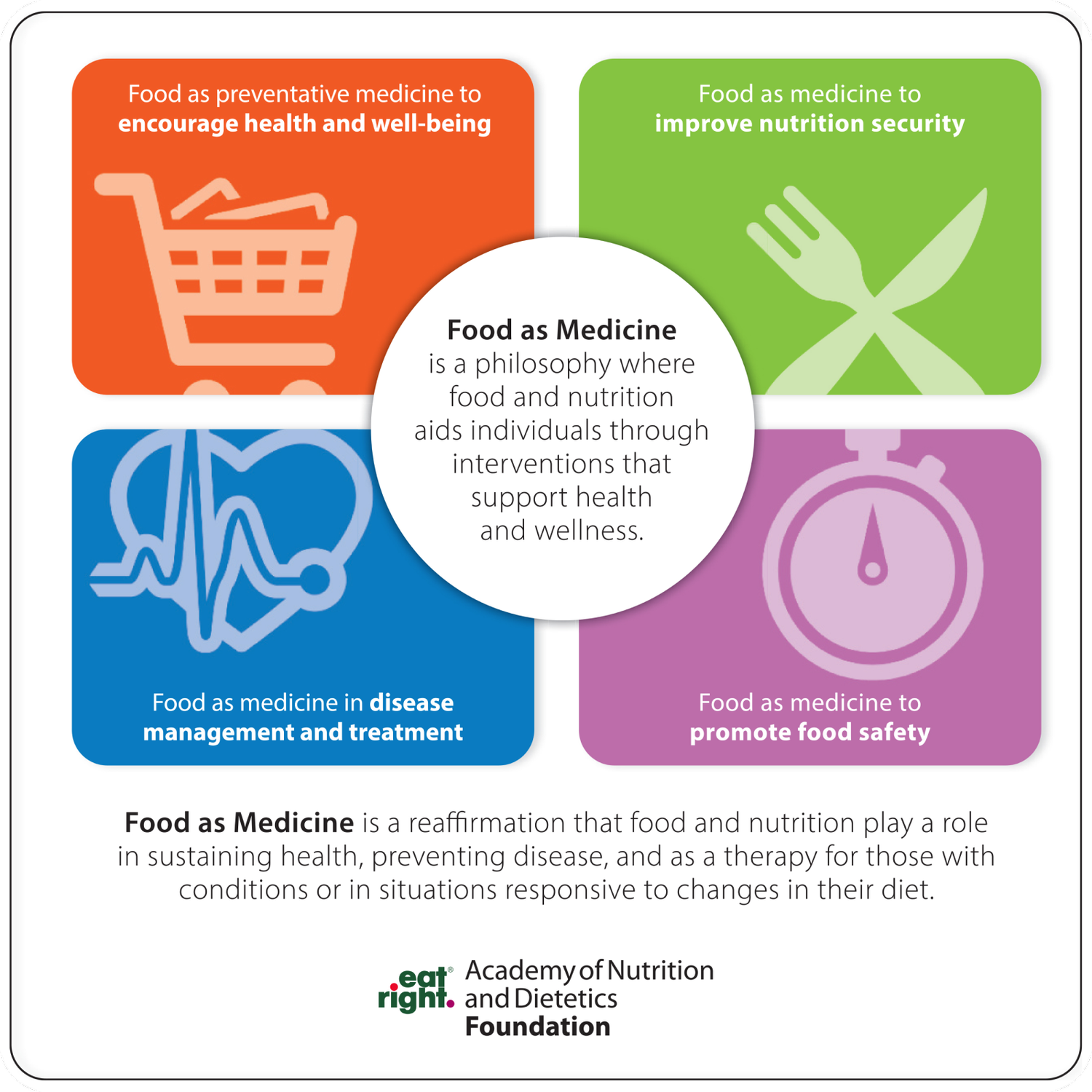
The new definition positions Food as Medicine (FAM) as “a philosophy where food and nutrition aids individuals through interventions that support health and wellness.”
By making FAM science-based, the Academy ensures that interventions are rigorously studied and medically-sound. They require more than a single, limited study. FAM dietary interventions are based on principles proven through precise, in-depth examination and analysis of the effects specific foods and diets have on people’s health.
While FAM plays a role in managing chronic conditions, and in some cases preventing or delaying them, it is clearly not intended to replace traditional medical care. The Academy frames FAM as complementing traditional medicine and doesn’t argue that FAM replaces it.
With its umbrella approach, the Academy avoids labeling any particular food or food group as “good” or “bad.” Instead, they endorse a more inclusive approach that avoids excluding or marginalizing foods less familiar in the Western diet. Limits can be recommended for foods known to encourage progression of a chronic condition. Yet, FAM doesn’t suggest eliminating any particular food or food group. FAM keeps the focus on supporting overall health along with a person’s individualized health and wellness needs — including satisfying the emotional and mental health needs that heritage and comfort food can address.
Source: Academy of Nutrition and Dietetics Foundation
In further discussing FAM, the Academy identifies four focus areas:
-
Food as preventative medicine to encourage health and well-being
-
Food as medicine in disease management and treatment
-
Food as medicine to improve nutrition security
-
Food as medicine to promote food safety
FAM in Disease Management and Treatment
Applying FAM principles to disease management and treatment once the chronic condition is diagnosed is not a new idea. We’re all likely familiar with dietary guidelines for particular diseases and conditions. Dietary recommendations for diabetes, kidney disease, and heart disease have all been widely promoted.
However, FAM can be extended to address prevention and slowing progression of some chronic conditions. Those conditions, whose progression is driven largely by dietary and nutritional factors, are strong candidates for applying FAM early on when a person’s risk level is identified and well before a formal diagnosis is made.
As we learn more about how chronic conditions start and progress, the more effective predictive medicine becomes. New tests and techniques can be developed to uncover an individual’s risk level early on — before signs, symptoms, or organ damage appear.
What’s more, as we get better at identifying individual risk levels and anticipating how chronic conditions progress, personalized medicine can begin to replace the one-size-fits-all approach that is so common today.
Looking Ahead
Embracing the FAM approach offers us a glimpse into the future of healthcare. It opens up a whole new realm where personalized and medically-customized nutrition works hand in hand with predictive health screenings like NaviDKD® to steer us away from the path of chronic conditions and their relentless progression.
NaviDKD Enables FAM in Diabetes & Kidney Care
NaviDKD, our flagship screening, analyzes blood biomarkers to assess kidney disease risk in people with diabetes. This enables healthcare professionals and people with diabetes to proactively manage and prevent the onset of diabetes-related kidney disease, ultimately improving health outcomes.
NaviDKD is unique in the fact that it identifies risk long before any signs or symptoms are present. This early warning provides the person with the time and understanding needed to effectively take actions that preserve or improve their own kidney health.
To learn more about NaviDKD, contact us.
About Journey Biosciences
Journey Biosciences is on a mission to improve the lives of people with diabetes through proactive, personalized care. One in three people with diabetes faces the hidden threat of kidney disease. Our flagship solution, NaviDKD®, is an innovative blood test that identifies this risk years in advance, enabling personalized preventive care for better health outcomes. By empowering early action, we aim to significantly reduce the burden of diabetes-related kidney disease on patients and healthcare systems. Discover more at journeybio.life.
For media inquiries: media@journeybio.life



